How Does AI Document Triage Work in Clinics?
Healthcare Technology
Healthcare Technology
AI document triage uses OCR and NLP to digitize, classify, extract, and route clinical documents, speeding workflows, reducing errors, and prioritizing urgent cases.
AI document triage uses OCR and NLP to digitize, classify, extract, and route clinical documents, speeding workflows, reducing errors, and prioritizing urgent cases.

AI document triage uses OCR (Optical Character Recognition) and NLP (Natural Language Processing) to handle clinical documents like referrals, lab results, and prior authorizations. It automates tasks such as classifying, extracting key details (e.g., patient names, diagnosis codes), and routing documents, reducing manual work and prioritizing urgent cases.
Key Takeaways:
Why It’s Needed: Clinics deal with high volumes of documents daily. Manual processing causes delays, errors, and compliance risks.
How It Works:
Digitization: Converts documents into machine-readable formats.
Classification: Sorts documents by type (e.g., lab results, referrals) and assigns priority.
Entity Extraction: Identifies critical details like patient info and urgency indicators.
Routing: Sends documents to the right staff or system based on urgency and type.
Integration: Works with EMR systems and complies with HIPAA and other security standards.
Benefits: Speeds up document handling, reduces human error, and frees up staff for patient care.
AI document triage is transforming how clinics manage administrative tasks, improving efficiency and reducing delays in patient care.
Core Components of AI Document Triage
Capture and Digitization
The first step is transforming clinical documents into a machine-readable format. This process takes unstructured data and converts it into a structured form, making it ready for analysis.
Document Classification and Priority Scoring
Once digitized, machine learning steps in to classify the documents - such as referrals, lab results, or prior authorizations. It also assigns priority scores based on clinical indicators and historical trends. For instance, documents mentioning acute symptoms or critical values are flagged as higher priority.
Entity Extraction and Routing
Natural Language Processing (NLP) is used to pull out essential details like patient names, birth dates, service dates, and diagnosis codes. These details are then matched to patient records in the EMR using a Master Patient Index. Depending on the urgency, the system routes documents accordingly - for example, urgent cases might go directly to a triage nurse, while prior authorizations are sent to billing. If the system is uncertain about any extraction, it flags those cases for human review, helping improve the model's accuracy over time. Together, these components create a streamlined workflow for clinics.
Accelerate referral processing with AI guided triage
Step-by-Step Workflow of AI Document Triage
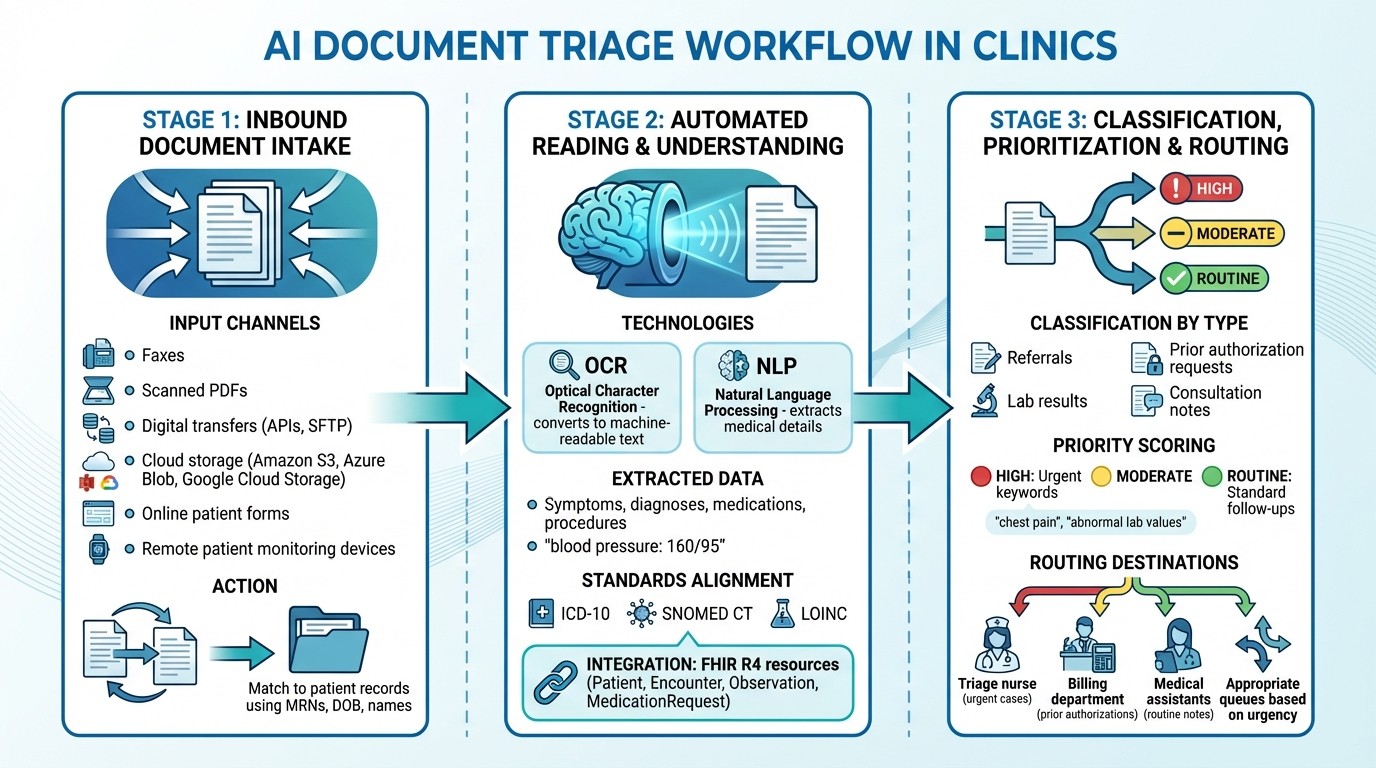
AI Document Triage Workflow: From Intake to Routing in Clinical Settings
Inbound Document Intake
Documents make their way into the clinic through multiple channels, including faxes, scanned PDFs, or digital transfers via APIs, SFTP, and cloud storage platforms like Amazon S3, Azure Blob, or Google Cloud Storage. Clinics also gather patient information through structured online forms, which may include checkbox responses and free-text fields for describing symptoms. For practices utilizing remote patient monitoring, the system can even handle real-time data from connected health devices.
Once received, the system matches these documents to patient records using identifiers like MRNs, dates of birth, and names. This process relies on patient indexing methods to ensure accurate matching before moving forward. After linking documents to the correct records, the system begins analyzing their content.
Automated Reading and Understanding
Next, the system uses OCR (optical character recognition) and layout analysis to transform various document formats into machine-readable text and images. From there, NLP (natural language processing) tools extract essential medical details, such as symptoms, diagnoses, medications, procedures, and structured data like key-value pairs (e.g., "blood pressure: 160/95" or "appointment date: 12/15/2025"). This information is then aligned with standard medical terminologies, including ICD-10, SNOMED CT, and LOINC, ensuring seamless integration with EMR systems through FHIR R4 resources like Patient, Encounter, Observation, and MedicationRequest.
Classification, Prioritization, and Routing
Once the content is processed, the AI classifies each document by type - such as a referral, lab result, prior authorization request, or consultation note - and assigns a priority score. Documents flagged with urgent keywords (e.g., "chest pain" or "abnormal lab values") are marked with higher priority compared to routine notes. Based on these classifications and priority levels, the system directs documents to the appropriate queues for further action.
Implementing AI Document Triage in Clinics
Assessing Current Workflows and Needs
Before introducing AI document triage, clinics need to take a close look at their existing workflows. Start by identifying where documents come from and where things tend to slow down. Track how many documents you handle daily, paying attention to peak times and the types of documents that create the biggest delays. For example, are referrals getting misrouted? Are urgent lab results being overlooked? Or is too much time spent manually sorting through faxes? Talking with staff can help uncover these administrative pain points. Another key step is reviewing how patient data is organized. AI models need access to labeled examples of your clinic’s actual documents - like referrals, prior authorization requests, and consultation notes - so they can learn your specific processes and terminology. Once you’ve mapped out these challenges, you can start customizing AI tools to meet your clinic’s needs.
Configuring AI Models and Rules
To make AI work for your clinic, you'll need to train the system using examples of the document types you handle every day. This involves feeding it samples of each category, along with details on how you currently prioritize and route them. For instance, you might set up the system to flag phrases like "chest pain" or "abnormal lab values" as urgent, ensuring they go to the right team immediately. Meanwhile, routine follow-up notes can be directed to medical assistants. The AI should also learn your clinic’s unique formats and terminology. To improve accuracy, have a human review low-confidence results and use that feedback to refine the system over time. This process ensures the AI adapts as your workflows evolve and maintains accuracy across various document types. Once the models and rules are fine-tuned, the next step is integrating them with your EMR system.
Ensuring Integration and Compliance
For AI document triage to be effective, it must integrate smoothly with your existing EMR system. Using HL7 v2 and FHIR R4 protocols allows seamless data exchange between the AI platform and your EMR, ensuring that extracted information automatically populates the correct fields without manual input. On the compliance front, it’s vital to confirm that your AI platform meets HIPAA requirements. Secure a Business Associate Agreement (BAA) before handling any Protected Health Information (PHI). Additionally, implement safeguards like encryption, role-based access control (RBAC), and immutable audit logs to protect patient data. For added security, consider isolating PHI within Virtual Private Clouds (VPCs) or using private endpoints. These measures not only protect sensitive information but also prepare your clinic for HIPAA audits and compliance checks.
Measuring Impact and Optimizing AI Triage
Once workflows are running smoothly, the next step is to measure the impact of AI triage and ensure it continues to improve patient care.
Key Metrics to Track
After implementation, it's essential to monitor specific metrics to evaluate performance. Start by measuring document processing time - compare how long it takes to route documents now versus before AI was introduced. Keep an eye on manual interventions, noting how often staff need to step in to correct AI decisions. Track error rates by identifying misclassifications or missed urgent cases. Another crucial metric is cost savings. For example, studies suggest that automating even a handful of administrative tasks in U.S. healthcare could save $13.3 billion. By optimizing workflows with AI, you can also reduce the administrative workload, which currently consumes up to 34% of staff time. Lastly, monitor staff satisfaction - their confidence and willingness to adopt the system are strong indicators of long-term success. These metrics not only show progress but also help refine the AI system based on real-world feedback.
Refining Models Through Feedback
AI systems thrive on feedback, and staff input plays a significant role in making improvements. At NYU Langone Health, for instance, biweekly feedback sessions with stakeholders helped fine-tune model thresholds, leading to better prioritization accuracy. Nurses reported increased trust in the system’s "High" priority labels and noted no critical errors in missing urgent messages. This AI model has been running for over a year and processes around 4,000 messages weekly. To keep improving, allow staff to flag issues anonymously, such as through surveys, and use this data to retrain your models. Regular retraining ensures the AI evolves alongside changes in workflows and document types.
Expanding Scope and Capabilities
Once the initial goals of AI triage are achieved, consider expanding its use to other administrative areas. Identify the next major bottleneck - this could be anything from appointment scheduling to managing patient intake forms or even supporting clinical decisions. The AI system should also be able to integrate data from various sources, such as specialty providers, labs, pharmacies, and insurers, to provide a more complete view of each patient. According to Gartner, by 2027, 60% of healthcare AI automation efforts will focus on addressing staff shortages and burnout, with generative AI potentially cutting clinical documentation time in half. As you broaden the scope, remain transparent and vigilant about issues like bias, and ensure compliance with data governance standards. Expanding step by step, while keeping staff engaged and confident in the system, will set the stage for ongoing success.
Conclusion: The Future of AI Document Triage in Clinics
AI document triage is reshaping how U.S. clinics manage the growing influx of patient data. With healthcare data increasing by nearly 36% each year, relying on manual processes is becoming impractical. Clinics that implement AI-powered automation experience tangible benefits, including a 30–60% reduction in manual data entry for specific documents, 20–40% faster prior authorization processes, and 10–20% fewer preventable denials. These improvements not only enhance efficiency but also help reduce costs, creating a foundation for tackling regulatory challenges.
The need for AI adoption is especially pressing in today’s heavily regulated healthcare environment. In 2023 alone, U.S. healthcare organizations reported 725 data breaches, impacting over 133 million records. Slava Khristich, CTO of TATEEDA GLOBAL, emphasized the urgency of this shift:
The operational and reputational cost makes automation and governance a survival topic, not a trend piece.
Between 2019 and 2023, 75% of U.S. healthcare providers increased their budgets for digital and IT initiatives, with more than 85% planning additional increases through 2024. Key priorities include cybersecurity and workflow automation.
Amid these challenges, ensuring HIPAA compliance remains a top concern. Secure AI platforms play a crucial role by offering full auditability and data traceability. These systems link every output field to its source, model version, and reviewer actions - features that are indispensable for audits and resolving disputes. Additionally, seamless integration with existing EHR/EMR systems through standards like HL7 v2 and FHIR R4 ensures that these advancements do not disrupt current workflows.
FAQs
How does AI document triage protect patient data and comply with HIPAA regulations?
AI document triage plays a critical role in safeguarding patient data while adhering to HIPAA regulations. It achieves this through robust security measures such as data encryption, role-based access controls, and secure authentication processes - designed to block unauthorized access effectively.
Moreover, these systems keep meticulous audit trails to monitor how data is used and ensure accountability. They also integrate smoothly with HIPAA-compliant platforms like HL7 and FHIR, creating a secure and efficient environment that protects sensitive information while enhancing clinical workflows.
What are the main advantages of using AI for document triage in clinics?
Introducing AI-powered document triage in clinics can bring a range of benefits. For starters, it can significantly cut down on administrative tasks by automating the sorting and prioritization of patient documents. This means staff can dedicate more time to what truly matters - delivering quality patient care.
AI also excels at improving accuracy when identifying urgent cases, ensuring that critical information doesn’t get overlooked and is handled promptly.
By simplifying workflows and integrating smoothly with EMR systems, clinics can improve efficiency and resource management. This can lead to shorter wait times and better care coordination, creating a more positive experience for both patients and healthcare providers.
How does AI document triage work with EMR systems in clinics?
AI document triage integrates effortlessly with existing EMR systems by transforming extracted data into standardized formats such as FHIR or HL7 v2. This guarantees precise integration and efficient routing of patient information where it’s needed.
The technology streamlines processes by automating tasks like classifying, prioritizing, and directing documents to the appropriate workflows. At the same time, it flags cases with low confidence for human review, ensuring accuracy. Additionally, it adheres to HIPAA regulations and generates detailed audit trails, boosting both operational efficiency and data security in clinical settings.
Related Blog Posts
AI document triage uses OCR (Optical Character Recognition) and NLP (Natural Language Processing) to handle clinical documents like referrals, lab results, and prior authorizations. It automates tasks such as classifying, extracting key details (e.g., patient names, diagnosis codes), and routing documents, reducing manual work and prioritizing urgent cases.
Key Takeaways:
Why It’s Needed: Clinics deal with high volumes of documents daily. Manual processing causes delays, errors, and compliance risks.
How It Works:
Digitization: Converts documents into machine-readable formats.
Classification: Sorts documents by type (e.g., lab results, referrals) and assigns priority.
Entity Extraction: Identifies critical details like patient info and urgency indicators.
Routing: Sends documents to the right staff or system based on urgency and type.
Integration: Works with EMR systems and complies with HIPAA and other security standards.
Benefits: Speeds up document handling, reduces human error, and frees up staff for patient care.
AI document triage is transforming how clinics manage administrative tasks, improving efficiency and reducing delays in patient care.
Core Components of AI Document Triage
Capture and Digitization
The first step is transforming clinical documents into a machine-readable format. This process takes unstructured data and converts it into a structured form, making it ready for analysis.
Document Classification and Priority Scoring
Once digitized, machine learning steps in to classify the documents - such as referrals, lab results, or prior authorizations. It also assigns priority scores based on clinical indicators and historical trends. For instance, documents mentioning acute symptoms or critical values are flagged as higher priority.
Entity Extraction and Routing
Natural Language Processing (NLP) is used to pull out essential details like patient names, birth dates, service dates, and diagnosis codes. These details are then matched to patient records in the EMR using a Master Patient Index. Depending on the urgency, the system routes documents accordingly - for example, urgent cases might go directly to a triage nurse, while prior authorizations are sent to billing. If the system is uncertain about any extraction, it flags those cases for human review, helping improve the model's accuracy over time. Together, these components create a streamlined workflow for clinics.
Accelerate referral processing with AI guided triage
Step-by-Step Workflow of AI Document Triage

AI Document Triage Workflow: From Intake to Routing in Clinical Settings
Inbound Document Intake
Documents make their way into the clinic through multiple channels, including faxes, scanned PDFs, or digital transfers via APIs, SFTP, and cloud storage platforms like Amazon S3, Azure Blob, or Google Cloud Storage. Clinics also gather patient information through structured online forms, which may include checkbox responses and free-text fields for describing symptoms. For practices utilizing remote patient monitoring, the system can even handle real-time data from connected health devices.
Once received, the system matches these documents to patient records using identifiers like MRNs, dates of birth, and names. This process relies on patient indexing methods to ensure accurate matching before moving forward. After linking documents to the correct records, the system begins analyzing their content.
Automated Reading and Understanding
Next, the system uses OCR (optical character recognition) and layout analysis to transform various document formats into machine-readable text and images. From there, NLP (natural language processing) tools extract essential medical details, such as symptoms, diagnoses, medications, procedures, and structured data like key-value pairs (e.g., "blood pressure: 160/95" or "appointment date: 12/15/2025"). This information is then aligned with standard medical terminologies, including ICD-10, SNOMED CT, and LOINC, ensuring seamless integration with EMR systems through FHIR R4 resources like Patient, Encounter, Observation, and MedicationRequest.
Classification, Prioritization, and Routing
Once the content is processed, the AI classifies each document by type - such as a referral, lab result, prior authorization request, or consultation note - and assigns a priority score. Documents flagged with urgent keywords (e.g., "chest pain" or "abnormal lab values") are marked with higher priority compared to routine notes. Based on these classifications and priority levels, the system directs documents to the appropriate queues for further action.
Implementing AI Document Triage in Clinics
Assessing Current Workflows and Needs
Before introducing AI document triage, clinics need to take a close look at their existing workflows. Start by identifying where documents come from and where things tend to slow down. Track how many documents you handle daily, paying attention to peak times and the types of documents that create the biggest delays. For example, are referrals getting misrouted? Are urgent lab results being overlooked? Or is too much time spent manually sorting through faxes? Talking with staff can help uncover these administrative pain points. Another key step is reviewing how patient data is organized. AI models need access to labeled examples of your clinic’s actual documents - like referrals, prior authorization requests, and consultation notes - so they can learn your specific processes and terminology. Once you’ve mapped out these challenges, you can start customizing AI tools to meet your clinic’s needs.
Configuring AI Models and Rules
To make AI work for your clinic, you'll need to train the system using examples of the document types you handle every day. This involves feeding it samples of each category, along with details on how you currently prioritize and route them. For instance, you might set up the system to flag phrases like "chest pain" or "abnormal lab values" as urgent, ensuring they go to the right team immediately. Meanwhile, routine follow-up notes can be directed to medical assistants. The AI should also learn your clinic’s unique formats and terminology. To improve accuracy, have a human review low-confidence results and use that feedback to refine the system over time. This process ensures the AI adapts as your workflows evolve and maintains accuracy across various document types. Once the models and rules are fine-tuned, the next step is integrating them with your EMR system.
Ensuring Integration and Compliance
For AI document triage to be effective, it must integrate smoothly with your existing EMR system. Using HL7 v2 and FHIR R4 protocols allows seamless data exchange between the AI platform and your EMR, ensuring that extracted information automatically populates the correct fields without manual input. On the compliance front, it’s vital to confirm that your AI platform meets HIPAA requirements. Secure a Business Associate Agreement (BAA) before handling any Protected Health Information (PHI). Additionally, implement safeguards like encryption, role-based access control (RBAC), and immutable audit logs to protect patient data. For added security, consider isolating PHI within Virtual Private Clouds (VPCs) or using private endpoints. These measures not only protect sensitive information but also prepare your clinic for HIPAA audits and compliance checks.
Measuring Impact and Optimizing AI Triage
Once workflows are running smoothly, the next step is to measure the impact of AI triage and ensure it continues to improve patient care.
Key Metrics to Track
After implementation, it's essential to monitor specific metrics to evaluate performance. Start by measuring document processing time - compare how long it takes to route documents now versus before AI was introduced. Keep an eye on manual interventions, noting how often staff need to step in to correct AI decisions. Track error rates by identifying misclassifications or missed urgent cases. Another crucial metric is cost savings. For example, studies suggest that automating even a handful of administrative tasks in U.S. healthcare could save $13.3 billion. By optimizing workflows with AI, you can also reduce the administrative workload, which currently consumes up to 34% of staff time. Lastly, monitor staff satisfaction - their confidence and willingness to adopt the system are strong indicators of long-term success. These metrics not only show progress but also help refine the AI system based on real-world feedback.
Refining Models Through Feedback
AI systems thrive on feedback, and staff input plays a significant role in making improvements. At NYU Langone Health, for instance, biweekly feedback sessions with stakeholders helped fine-tune model thresholds, leading to better prioritization accuracy. Nurses reported increased trust in the system’s "High" priority labels and noted no critical errors in missing urgent messages. This AI model has been running for over a year and processes around 4,000 messages weekly. To keep improving, allow staff to flag issues anonymously, such as through surveys, and use this data to retrain your models. Regular retraining ensures the AI evolves alongside changes in workflows and document types.
Expanding Scope and Capabilities
Once the initial goals of AI triage are achieved, consider expanding its use to other administrative areas. Identify the next major bottleneck - this could be anything from appointment scheduling to managing patient intake forms or even supporting clinical decisions. The AI system should also be able to integrate data from various sources, such as specialty providers, labs, pharmacies, and insurers, to provide a more complete view of each patient. According to Gartner, by 2027, 60% of healthcare AI automation efforts will focus on addressing staff shortages and burnout, with generative AI potentially cutting clinical documentation time in half. As you broaden the scope, remain transparent and vigilant about issues like bias, and ensure compliance with data governance standards. Expanding step by step, while keeping staff engaged and confident in the system, will set the stage for ongoing success.
Conclusion: The Future of AI Document Triage in Clinics
AI document triage is reshaping how U.S. clinics manage the growing influx of patient data. With healthcare data increasing by nearly 36% each year, relying on manual processes is becoming impractical. Clinics that implement AI-powered automation experience tangible benefits, including a 30–60% reduction in manual data entry for specific documents, 20–40% faster prior authorization processes, and 10–20% fewer preventable denials. These improvements not only enhance efficiency but also help reduce costs, creating a foundation for tackling regulatory challenges.
The need for AI adoption is especially pressing in today’s heavily regulated healthcare environment. In 2023 alone, U.S. healthcare organizations reported 725 data breaches, impacting over 133 million records. Slava Khristich, CTO of TATEEDA GLOBAL, emphasized the urgency of this shift:
The operational and reputational cost makes automation and governance a survival topic, not a trend piece.
Between 2019 and 2023, 75% of U.S. healthcare providers increased their budgets for digital and IT initiatives, with more than 85% planning additional increases through 2024. Key priorities include cybersecurity and workflow automation.
Amid these challenges, ensuring HIPAA compliance remains a top concern. Secure AI platforms play a crucial role by offering full auditability and data traceability. These systems link every output field to its source, model version, and reviewer actions - features that are indispensable for audits and resolving disputes. Additionally, seamless integration with existing EHR/EMR systems through standards like HL7 v2 and FHIR R4 ensures that these advancements do not disrupt current workflows.
FAQs
How does AI document triage protect patient data and comply with HIPAA regulations?
AI document triage plays a critical role in safeguarding patient data while adhering to HIPAA regulations. It achieves this through robust security measures such as data encryption, role-based access controls, and secure authentication processes - designed to block unauthorized access effectively.
Moreover, these systems keep meticulous audit trails to monitor how data is used and ensure accountability. They also integrate smoothly with HIPAA-compliant platforms like HL7 and FHIR, creating a secure and efficient environment that protects sensitive information while enhancing clinical workflows.
What are the main advantages of using AI for document triage in clinics?
Introducing AI-powered document triage in clinics can bring a range of benefits. For starters, it can significantly cut down on administrative tasks by automating the sorting and prioritization of patient documents. This means staff can dedicate more time to what truly matters - delivering quality patient care.
AI also excels at improving accuracy when identifying urgent cases, ensuring that critical information doesn’t get overlooked and is handled promptly.
By simplifying workflows and integrating smoothly with EMR systems, clinics can improve efficiency and resource management. This can lead to shorter wait times and better care coordination, creating a more positive experience for both patients and healthcare providers.
How does AI document triage work with EMR systems in clinics?
AI document triage integrates effortlessly with existing EMR systems by transforming extracted data into standardized formats such as FHIR or HL7 v2. This guarantees precise integration and efficient routing of patient information where it’s needed.
The technology streamlines processes by automating tasks like classifying, prioritizing, and directing documents to the appropriate workflows. At the same time, it flags cases with low confidence for human review, ensuring accuracy. Additionally, it adheres to HIPAA regulations and generates detailed audit trails, boosting both operational efficiency and data security in clinical settings.